Specialized HVAC Systems in Dental Clinics: An Emerging Necessity for Infection Control & Indoor Air Quality
Abstract
The rapid growth of organized dental clinics in urban environments, along with increasing procedural specialization, has significantly elevated the importance of engineered HVAC systems. Beyond thermal comfort, these systems are now integral to infection control, indoor air quality (IAQ), and occupational safety.This article highlights the risks associated with inadequate HVAC design in dental settings and outlines key engineering considerations for creating safer clinical environments.
Introduction
Dental clinics have evolved from basic treatment spaces into highly specialized healthcare environments. However, HVAC design in many facilities still follows a comfort-centric approach rather than a clinical one.This gap exposes patients, dentists, and healthcare workers to preventable risks related to poor air quality and airborne infection transmission.
Air Quality Concerns in Dental Procedures
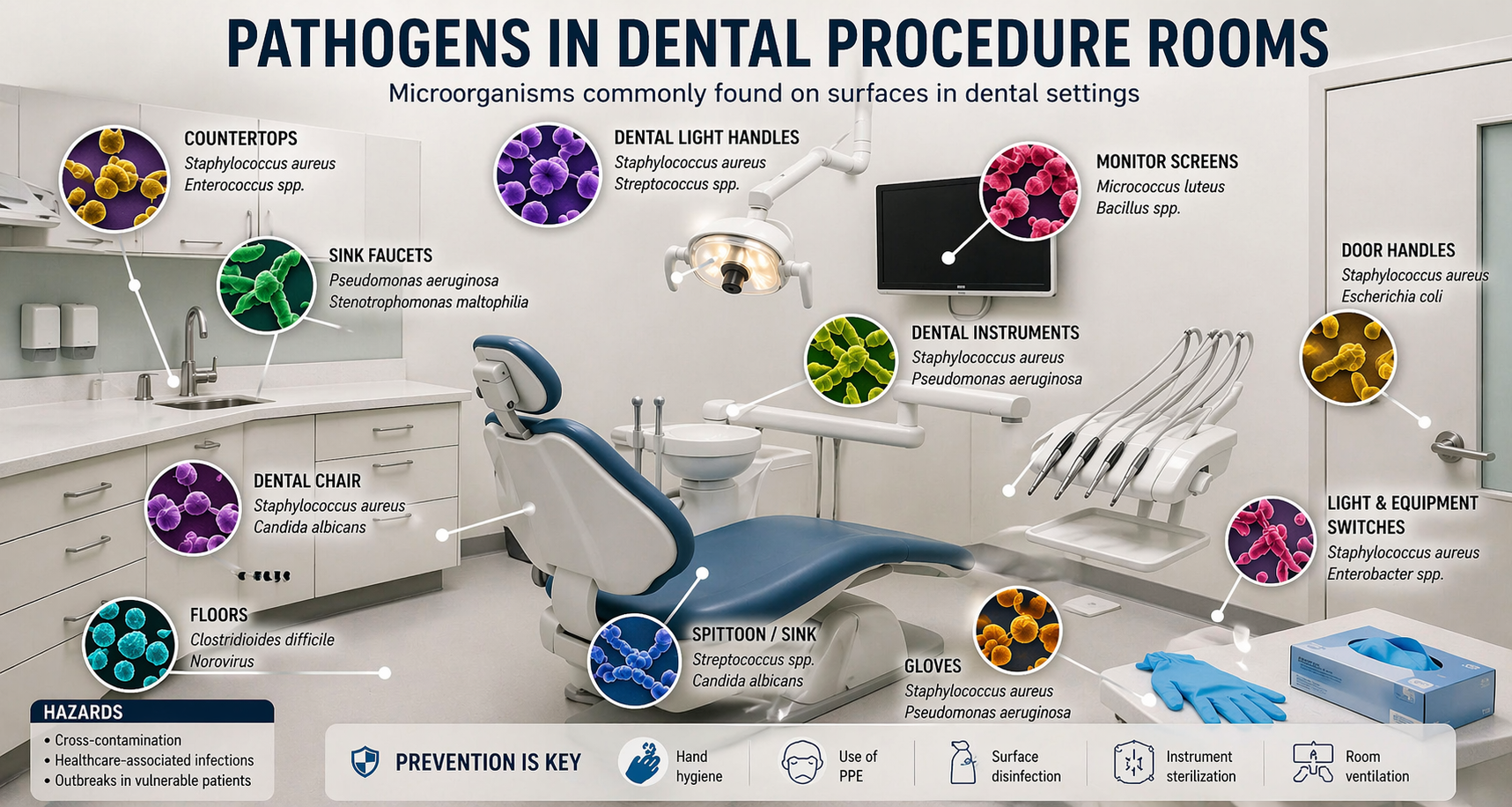
Dental treatments inherently generate airborne contaminants. Procedures such as drilling, grinding, and polishing produce aerosols and fine particulate matter (PM2.5). Additionally, dental materials used in restorative and cosmetic procedures emit volatile organic compounds (VOCs), contributing to indoor air pollution.Studies indicate that: • Dental clinics often have elevated levels of respirable particulate matter • Aerosols generated during procedures may carry microbial contaminants • VOC emissions can accumulate in poorly ventilated spacesThese factors collectively degrade indoor air quality and pose both short-term and long-term health risks.
Infection Control & Airborne Risks
In the post-pandemic era, infection prevention in dental clinics has become even more critical. Aerosol-generating procedures significantly increase the risk of airborne transmission.Key concerns include: • Exposure to pathogen-laden aerosols • Increased vulnerability for immunocompromised individuals • Higher chances of cross-contamination in poorly ventilated roomsIn such environments, HVAC systems act as a primary engineering control to mitigate these risks.
Key HVAC Engineering Considerations
While region-specific regulations are still evolving, global healthcare guidelines and ASHRAE recommendations provide a strong foundation.Critical design factors include:
• Ventilation: Minimum 6 Air Changes per Hour (ACH)
• Pressure Control: Negative pressure in treatment rooms; positive pressure in clean zones
• Filtration: MERV-13 or HEPA filters for effective particle removal
• Airflow Direction: From clean to less clean areas
• UVGI Systems: For inactivation of airborne microorganisms
• Fresh Air & Exhaust: Balanced supply and exhaust for IAQ control
• Localized Air Cleaning: Portable HEPA units for high-risk areas
Limitations of Conventional Cooling Systems
Many dental clinics still rely on split air-conditioning systems designed only for thermal comfort. These systems lack fresh air integration, filtration, and contaminant removal capabilities.As a result, polluted indoor air continues to recirculate—creating environments that appear clean but may contain high levels of airborne contaminants.
Discussion
Dental clinics represent a unique healthcare segment where high aerosol generation meets prolonged exposure. Despite this, HVAC design is often underestimated and under-regulated.A shift toward performance-driven, healthcare-aligned engineering solutions is essential to bridge this gap.
Conclusion
As dental practices continue to advance, supporting infrastructure must evolve accordingly. HVAC systems are no longer auxiliary—they are critical to clinical safety and performance.Implementing scientifically designed ventilation, filtration, and air distribution systems is essential to: ✔ Protect patients ✔ Safeguard healthcare professionals ✔ Meet emerging global health standards
Clean air in dental clinics is not just about comfort—it is a necessity for safe and effective healthcare delivery.
